Common Orthopedic Disorders
Orthopedic disorders encompass a wide range of conditions affecting the musculoskeletal system, including bones, joints, ligaments, tendons, and muscles. These disorders can result from trauma, degenerative processes, congenital abnormalities, or systemic diseases. This review highlights the most prevalent orthopedic conditions, their etiology, clinical presentation, diagnostic approaches, and management strategies. The disorders discussed include osteoarthritis, osteoporosis, fractures, rotator cuff injuries, and spinal disorders such as herniated discs and scoliosis.
The musculoskeletal system is essential for mobility, stability, and overall quality of life. Orthopedic disorders are among the leading causes of disability worldwide, contributing significantly to healthcare burdens.
1. Osteoarthritis (OA)
Etiology and Pathophysiology
Osteoarthritis is the most common form of arthritis, characterized by the progressive degeneration of articular cartilage. Risk factors include aging, obesity, joint trauma, and genetic predisposition. The breakdown of cartilage leads to joint inflammation, pain, and stiffness.
Clinical Presentation
Patients typically experience joint pain, tenderness, and reduced range of motion. Commonly affected joints include the knees, hips, and hands.
Diagnosis
Diagnosis is primarily clinical, supported by imaging studies such as X-rays, which show joint space narrowing, osteophytes, and subchondral sclerosis.
Management
Treatment includes lifestyle modifications (e.g., weight loss, exercise), pharmacologic interventions (e.g., NSAIDs, acetaminophen), and surgical options (e.g., joint replacement) in severe cases.
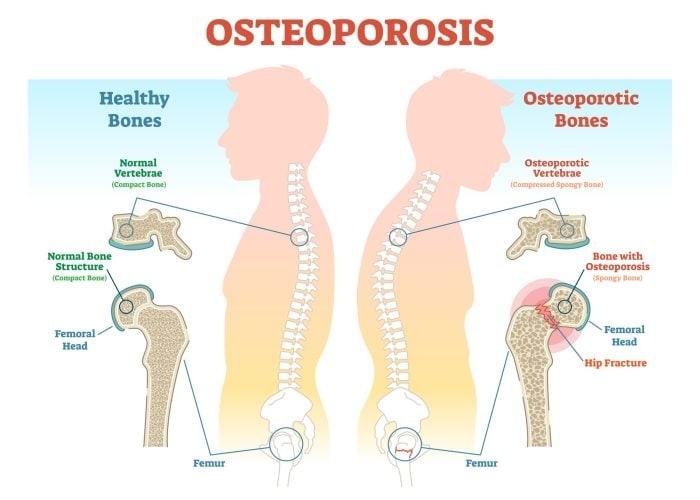
2. Osteoporosis
Etiology and Pathophysiology
Osteoporosis is a systemic skeletal disorder characterized by reduced bone mass and microarchitectural deterioration, leading to increased fracture risk. It is often associated with aging, hormonal changes (e.g., menopause), and nutritional deficiencies (e.g., calcium, vitamin D).
Clinical Presentation
Osteoporosis is often asymptomatic until a fracture occurs. Common fracture sites include the hip, spine, and wrist.
Diagnosis
Bone mineral density (BMD) testing via dual-energy X-ray absorptiometry (DXA) is the gold standard for diagnosis.
Management
Treatment focuses on fracture prevention through calcium and vitamin D supplementation, bisphosphonates, and lifestyle changes such as weight-bearing exercises.
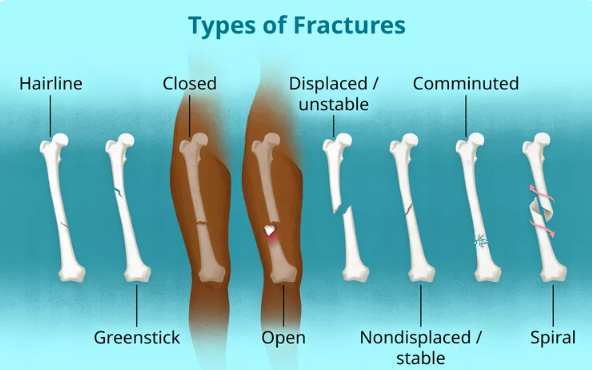
3. Fractures
Etiology and Pathophysiology
Fractures result from traumatic injuries or pathological conditions (e.g., osteoporosis, bone tumors). They are classified based on location, pattern, and displacement.
Clinical Presentation
Symptoms include pain, swelling, deformity, and loss of function at the fracture site.
Diagnosis
Diagnosis is confirmed through imaging studies, including X-rays, CT scans, or MRIs.
Management
Treatment involves immobilization (e.g., casting, splinting), reduction, and surgical fixation (e.g., internal or external fixation) for complex fractures.
4. Rotator Cuff Injuries
Etiology and Pathophysiology
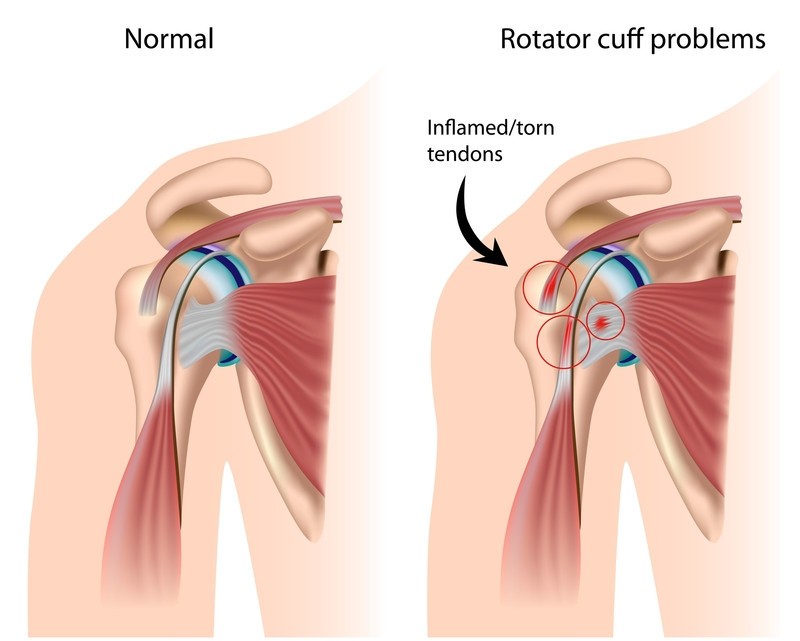
Rotator cuff injuries are common shoulder disorders caused by acute trauma or chronic degeneration. The rotator cuff tendons (supraspinatus, infraspinatus, teres minor, and subscapularis) are prone to tears and tendinitis.
Clinical Presentation
Patients report shoulder pain, weakness, and limited range of motion, particularly during overhead activities.
Diagnosis
Physical examination and imaging (e.g., MRI, ultrasound) are used to confirm the diagnosis.
Management
Treatment includes rest, physical therapy, corticosteroid injections, and surgical repair for severe tears.
5. Spinal Disorders
Herniated Disc
A herniated disc occurs when the nucleus pulposus protrudes through the annulus fibrosus, often compressing adjacent nerve roots. Symptoms include radicular pain, numbness, and weakness. Diagnosis is confirmed via MRI, and treatment ranges from conservative measures (e.g., physical therapy) to surgical intervention (e.g., discectomy).
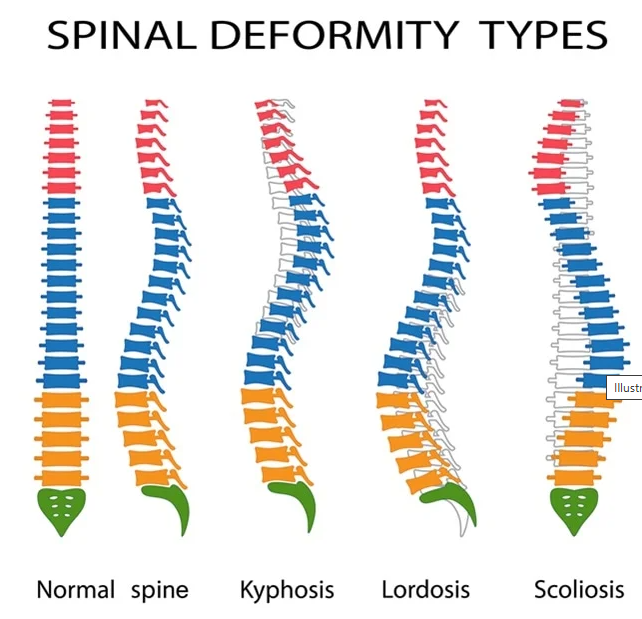
Scoliosis
Scoliosis is an abnormal lateral curvature of the spine, often idiopathic in adolescents. Severe cases can lead to respiratory and cardiovascular complications. Diagnosis is based on clinical examination and imaging (e.g., X-rays). Treatment includes bracing and spinal fusion surgery for progressive curves.
Conclusion
Orthopedic disorders are prevalent and significantly impact patients’ quality of life. Early diagnosis and appropriate management are crucial to prevent complications and improve outcomes. Advances in diagnostic imaging, minimally invasive surgical techniques, and regenerative therapies continue to enhance the treatment landscape for these conditions.
References
While I cannot provide direct citations, the following sources are commonly referenced in orthopedic literature:
- American Academy of Orthopaedic Surgeons (AAOS) Guidelines
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS)
- Journal of Bone and Joint Surgery (JBJS)
- Orthopedic Clinics of North America
- Textbooks: Campbell’s Operative Orthopaedics, Netter’s Orthopaedic Clinical Examination


